September 01, 2020 - by Simone Ulmer
The delicate valves of the human heart are an impressive anatomical masterpiece: the small, sail-like structures ensure the orderly flow of blood through the heart to the rest of the body. Healthy valves guide the blood so skilfully that it maintains a mostly laminar flow with no turbulence. However, pathological changes or congenital deformities in the heart valves can impair the bloodstream and thus the optimal blood flow. A defective aortic valve, for example, may lead to an aneurysm – a life-threatening event where the misdirected blood broadens and thins out the arterial wall until it eventually ruptures.
In order to prevent an aortic aneurysm, the defective heart valve can be replaced with a biological or mechanical valve. However, biological replacement valves have a limited lifespan of about 10 to 20 years, and it has not yet been possible to develop mechanical heart valves that can regulate blood flow as well as a natural one. Unfortunately, mechanical valves cause turbulence that leads to blood platelets clumping together and forming blood clots on the vessel walls. If these clots detach and move towards the brain, they may obstruct blood vessels and cause a stroke. As a result, patients with mechanical heart valves have to take blood thinners for the rest of their lives.
Turbulence caused by mechanical heart valves
Dominik Obrist, professor and head of the research group for Cardiovascular Engineering at the ARTORG Center for Biomedical Engineering Research at the University of Bern, has been investigating turbulent flow behaviour since 1996 – since working on his master’s thesis at ETH Zurich. Supercomputing resources at the CSCS are essential to this research. Today, Obrist also operates an experimental flow laboratory with cutting-edge measurement technology – a heartfelt wish the researcher was able to fulfil using his professorship funds seven years ago. The Aargau native is proud to show the equipment he and his team constructed themselves to investigate, among other things, the turbulence that occurs when the blood stream hits an artificial heart valve. In this experiment, a mixture of glycerine and water is used to simulate the blood flow. High-speed cameras and laser-based methods for three-dimensional flow quantification show what subsequently happens when the flow encounters the mechanical valve.
What is real?
The combination of simulation and experiment is important, Obrist explains, because running calculations and getting results does not necessarily reflect reality. “We computer people are good at taking partial differential equations, translating them into computer programmes and getting them to run. But we lack an understanding of biological processes.” Afterall, the anatomy of every human is different. This seems trivial at first, says Obrist, but when you build an aeroplane, the blueprint includes tolerances that guarantee that the wing lies within 0.1 mm above or below a specific length. “We know roughly the shape and size of a heart. The word ‘roughly’, however, reflects a mindset with which we as engineers struggle, as we have always learned that things must be precise,” he explains. In biology, everything is suddenly softer and difficult to grasp. Translating this into computer models is difficult, and Obrist is convinced that therefore experiments form a key complementary tool.
On this basis, he and his team were recently able to show what happens when blood meets a mechanical valve – particularly where and how the dangerous turbulence forms. Using this knowledge, heart valves could be optimised in a way that prevents the generation of turbulence altogether. For many people – 250,000 patients around the world receive a new valve every year – this may mean they would no longer need to take blood thinners, which could improve their quality of life.
A research career with detours
At the beginning of his career, it never occurred to Obrist that he would one day use his engineering expertise in medical research, particularly to investigate blood circulation with a special focus on heart valves. He took several professional detours before getting there. One of these initially led him to the University of Washington in Seattle, where he obtained his doctorate on fluid dynamics through research. However, his funding ran out before he could complete his work. Luckily, an internship at Tera Computer (which later became the supercomputer manufacturer Cray) led to a scholarship with which he could continue financing his doctoral thesis.
After two years in Seattle, Obrist’s son was born. He and his wife, who moved with him to Seattle, now wanted to return to Europe. “The US is cool for a young couple, but not with children. At the time, I had also had quite enough of the academic world,” he admits openly. “A young family and no money – I wanted to earn a proper salary.”
During his doctoral studies, Obrist had conducted research visits at the Technical University of Munich and the Leibniz Supercomputing Centre in Munich. Cray eventually offered him a steady role in Europe, and at first, he enjoyed the many trips as a pre-sales analyst and then an account manager. However, he eventually began to feel as though he were sitting on the wrong side of the negotiating table when he met researchers. It was therefore a crucial turning point for him when he met a former professor on one of his trips to Munich, who asked Obrist what he now did for a living. At the conference table in his office in Bern, Obrist mimics the way the shaken professor had to sit down under the weight of Obrist's confession that he now sold computers, saying to him half-jokingly: “Mr. Obrist, how low you have fallen.”
When he turned 35, it became clear: “Now is the last opportunity to switch to the other side of the table.” Luckily, ETH Zurich professor Leonhard Kleiser happened to have a vacancy at this time that launched Obrist’s career as a biomedical fluid mechanics engineer. Looking back, he is glad about his naivety – the difficulty he faced in returning to research after five years in industry and living on a senior researcher's salary again only became clear once it was too late to turn back.
Engineers as part of the medical faculty
About 15 years later, Obrist now conducts research in a state-of-the-art building within walking distance of the Inselspital, Bern University Hospital. As his institution is part of the medical faculty, he is convinced that the position he has today is unique in Switzerland, with barely anything similar worldwide. He is proud of his close collaboration with medicine and the direct exchange with doctors, who sometimes take him along to the operating room. There, they can outline specific issues live with a patient, or his team can take measurements and collect data from the patient during surgery. It is also not uncommon for doctors to call him with a question, which then turns into a project. This translation is routine within Obrist's work group, i.e. developing an idea discussed at the operating table or between the doctor and engineer, using it as the basis for a simulation and experiment, and then engineering it into a technical solution – a product. “I always wanted a professorship because I wanted the freedom to test things out,” says the professor.
Everything started to fall into place for him in 2005 when he came back to work at ETH Zurich and started a project on the inner ear and the sense of balance. “The inner ear was my ticket to the world of biomedical fluid mechanics,” says Obrist. In addition, he took over the biofluid dynamics lecture at ETH Zurich in 2006, a responsibility he still holds today. His research eventually led him to the heart because this is the most prominent area for flows in the body. Still, the flow of blood in the lungs, ear and brain were and remain part of his research portfolio, and a lot of heart research can also be translated to the urinary tract, he says. This is why the 48-year-old recently established a research group and a start-up in the field of urology, with a focus on stents for the ureter between the kidney and bladder. These often become encrusted, leading to problems, and the new team is researching the cause behind this issue.
Although Obrist has moved away from conventional mechanical engineering in the course of his career, he has remained faithful to the simulation of flow processes and thus to supercomputers. Even as a teenager, in addition to his passion for gliding – for which he obtained his license at the age of 17 and subsequently became one of the best glider pilots in Switzerland – he had a strong affinity for computers. At that time, he was not familiar with the term “computational science”, but he knew he wanted to study computer science. He is still not entirely sure how he ended up in mechanical engineering – it was a somewhat spontaneous decision when applying for his studies, but one that he has never regretted.
Long-term CSCS user
As a long-term user of supercomputers with a wide range of architectures within the CSCS infrastructure, Obrist now enjoys making the most of interdisciplinary research initiatives such as the Platform for Advanced Scientific Computing (PASC). “The technological changes to CSCS were initially a source of anguish for us, particularly the switch from vector processors to massively parallel computer architectures,” admits Obrist. However, when an adjusted code is suddenly able to run 1,000 times faster, he is happy to accept the technological leadership.
In PASC, he is currently working with computer scientists, doctors and medical imaging experts on the project “HPC-PREDICT – High-Performance Computing for the Prognosis of Adverse Aortic Events” to develop software for an innovative prognosis tool for disorders of the ascending aorta, specifically by improving the precision and accuracy of the image data. Dominik Obrist seemingly never runs out of research ideas. In fact, sometimes he worries that his spectrum is becoming a little too wide – but then he recognises that this variety precisely reflects the freedom he has always wanted.
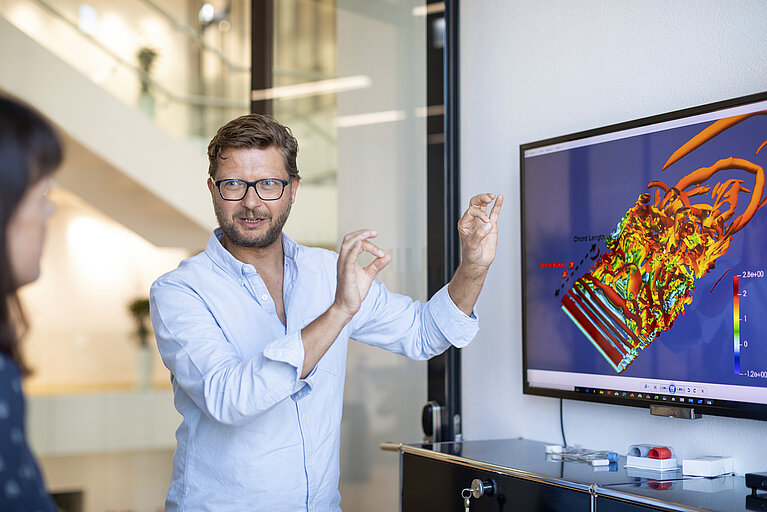
Image above: Since 2013 Dominik Obrist is professor at the ARTORG Center for Biomedical Engineering Research at the University of Bern. (Image: Alessandro Della Bella)
More information:
Latest research results of the research group for Cardiovascular Engineering at the ARTORG Center for Biomedical Engineering Research: Turbulent systolic flow downstream of a bioprosthetic aortic valve: velocity spectra, wall shear stresses and turbulent dissipation rates.
This article may be used on other media and online portals provided the copyright conditions are observed.